Florida Health Insurance Plans: Complete 2026 Guide
Compare plan types (HMO, PPO, EPO), coverage levels (Bronze through Platinum), top carriers, and costs. This guide walks through every aspect of choosing health coverage in Florida for 2026.
Understanding Florida Health Insurance Plans in 2026
Florida health insurance plans fall into two categories that together determine coverage and cost: the plan type (HMO, PPO, EPO, or POS) controls how care is accessed, while the metal tier (Bronze, Silver, Gold, or Platinum) sets the cost-sharing ratio. According to CMS 2025 Open Enrollment data, approximately 4.7 million Floridians enrolled through HealthCare.gov—the highest enrollment of any state in the country.
Selecting a plan type determines which doctors and hospitals are available, whether specialist referrals are required, and whether out-of-network visits are covered. The metal tier then sets the balance between monthly premiums (your regular payment to keep coverage active) and out-of-pocket costs like deductibles (what you pay before insurance kicks in) and copays (fixed fees per visit).
Sixteen carriers are offering Florida marketplace plans for 2026, with plan availability varying by county. Aetna exited the Florida marketplace at the end of 2025, while 22 Health (Community Care Network) entered as a new carrier serving Broward County. This guide covers both plan types and metal tiers in detail, plus costs, carrier options, and a step-by-step framework for choosing the right coverage.
Florida Health Insurance Marketplace: How It Works
The Florida Health Insurance Marketplace operates through HealthCare.gov, where residents shop for individual and family coverage, compare plans side by side, and apply for financial assistance. Open Enrollment for 2026 ran from November 1, 2025, through January 15, 2026, with coverage starting January 1 for those who enrolled by December 15. Starting in fall 2026, the enrollment window will shorten—ending December 15 instead of January 15.
Special Enrollment Periods remain available year-round for qualifying life events such as marriage, the birth or adoption of a child, loss of other coverage, or a move to a new state. All marketplace plans must cover the ten essential health benefits mandated by the Affordable Care Act, including ambulatory services, emergency care, hospitalization, maternity and newborn care, mental health and substance use services, prescription drugs, rehabilitative services, lab work, preventive care, and pediatric dental and vision.
Financial Assistance for 2026
Premium Tax Credits are available for individuals and families with incomes between 100% and 400% of the Federal Poverty Level. For 2026, that translates to $15,650–$62,600 for an individual or $32,150–$128,600 for a family of four. Earning even $1 over 400% FPL now means losing all subsidies—the cliff has returned after the enhanced credit expiration.
Cost-Sharing Reductions (CSRs) lower deductibles, copays, and coinsurance for Silver plan enrollees with incomes under 250% FPL ($39,125 for an individual, $80,375 for a family of four). CSRs are exclusive to Silver plans—choosing any other metal tier forfeits this benefit. For a deeper look at saving money on Florida coverage, the affordable health insurance Florida guide provides additional detail.

Florida Health Plan Types: HMO, PPO, EPO, and POS Compared
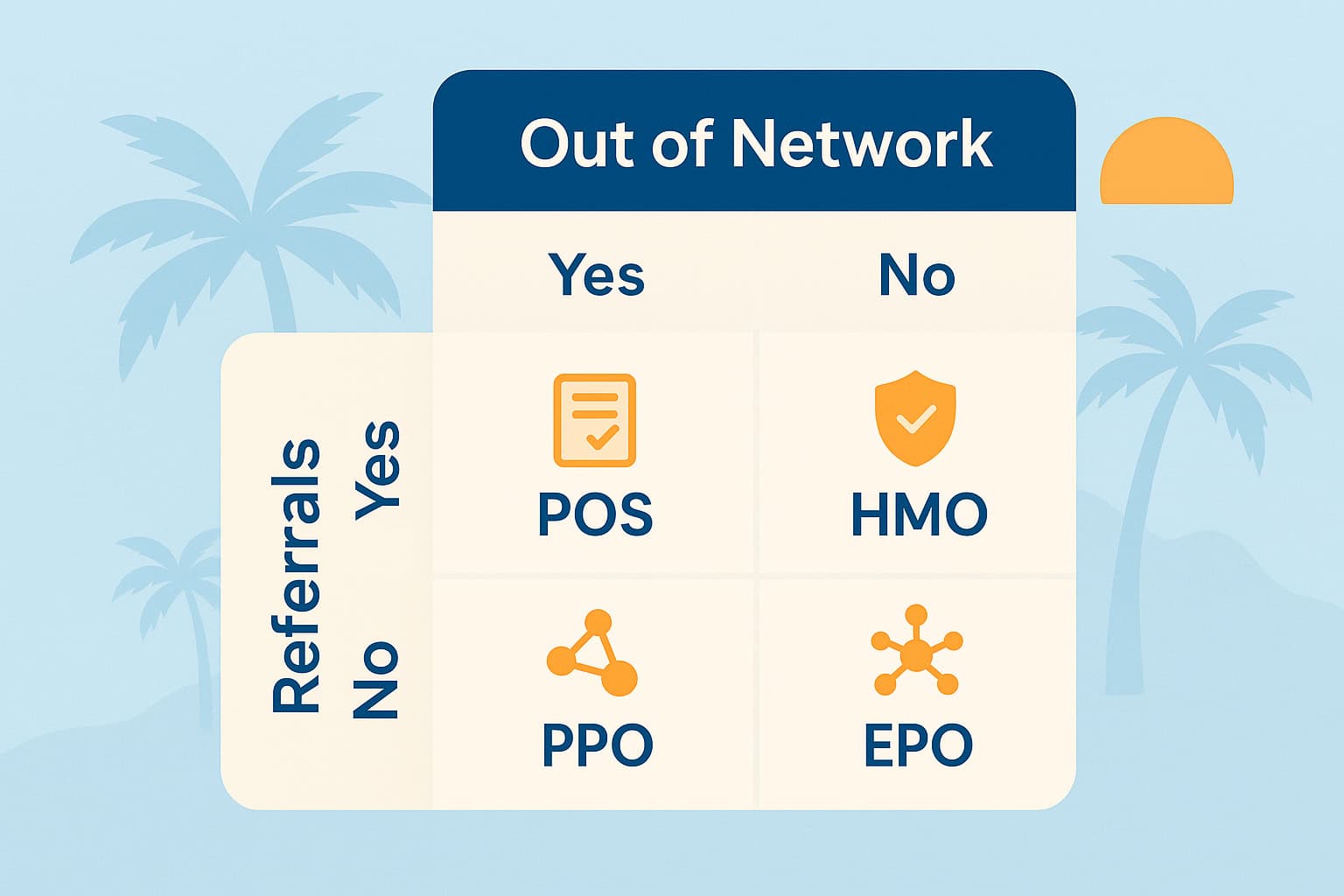
Four plan types are available through the Florida marketplace, each with distinct trade-offs between cost, flexibility, and administrative requirements. HMO plans carry the lowest premiums but require referrals and in-network-only care. PPO plans offer maximum flexibility at the highest premium cost. EPO and POS plans split the difference in different ways.
HMO Plans
Choose a primary care physician (PCP) who coordinates all care and provides referrals to specialists. Only in-network providers are covered except in emergencies.
Best for: Budget-conscious residents comfortable coordinating through a PCP and staying in-network.
PPO Plans
See any provider without referrals. In-network visits cost less, but out-of-network care is still partially covered. Premiums run 20–40% higher than comparable HMOs.
Best for: Those who want maximum flexibility, see multiple specialists, or travel frequently.
EPO Plans
See any in-network provider without referrals. No out-of-network coverage except emergencies. Combines HMO-level pricing with PPO-like freedom within the network.
Best for: Residents who want specialist access without referrals and are comfortable staying in-network.
POS Plans
Hybrid of HMO and PPO. Requires a PCP and referrals for in-network specialists, but allows out-of-network visits at higher cost.
Best for: Those who prefer PCP coordination but want occasional out-of-network flexibility.
Narrow Network Plans
Smaller provider networks in exchange for the lowest possible premiums. Structure varies—some function like HMOs, others like EPOs.
Best for: Residents whose preferred doctors are included and who prioritize the lowest monthly cost.
Choosing a Plan Type
Consider how often specialists are needed, whether provider freedom matters, monthly budget constraints, travel frequency, and how important out-of-network access is.
Tip: Most Florida residents choose HMO or EPO plans for the best value-to-coverage ratio.
For those who need maximum provider choice or who travel between states regularly, the Florida PPO health insurance guide covers PPO-specific options in greater detail.
Compare Florida Health Insurance Plan Types
Different plans serve different situations. Comparing options side by side helps identify the coverage that aligns with specific healthcare needs and budget.
Compare Plans Online Call 888-215-4045
Florida Health Plan Metal Tiers: Bronze Through Platinum
All marketplace plans are organized into four metal tiers—Bronze, Silver, Gold, and Platinum—based on the percentage of healthcare costs the plan covers on average. Metal tiers do not reflect care quality; they only determine how costs split between the enrollee and the insurance company. A Bronze plan covers approximately 60% of costs, while Platinum covers 90%.
Bronze Plans
Plan pays 60% | You pay 40%
Lowest premiums, highest deductibles (typically $6,000–$9,100+). Best for healthy individuals who primarily want emergency protection and the lowest monthly cost.
Silver Plans
Plan pays 70% | You pay 30%
Moderate premiums, medium deductibles ($3,000–$6,000). Best value for most people. The only tier eligible for Cost-Sharing Reductions, which can lower the deductible to under $1,000 for qualifying incomes.
Gold Plans
Plan pays 80% | You pay 20%
Higher premiums, lower deductibles ($1,000–$3,000). Best for those with chronic conditions, regular care needs, or anticipated medical expenses during the plan year.
Platinum Plans
Plan pays 90% | You pay 10%
Highest premiums, lowest deductibles ($0–$1,500). Best for those with significant ongoing medical needs, frequent care, or high expected healthcare costs.
Top Insurance Companies Offering Florida Plans in 2026
Sixteen carriers participate in Florida’s 2026 marketplace—the largest insurer pool of any HealthCare.gov state. Florida Blue remains the dominant carrier by enrollment and network size, while Ambetter, Oscar, Molina, and Cigna offer competitive alternatives in many counties. Carrier availability varies significantly by location; not all carriers serve all 67 counties.
| Feature | Flexible Network Plans (PPO/EPO) | HMO Plans |
|---|---|---|
| Monthly Premium (Typical) | $50–$150 more per month | Lower |
| Specialist Referrals | Not required | Required for most specialists |
| Out-of-Network Coverage | Yes (PPO) or No (EPO), at higher cost | Emergency only |
| Primary Care Doctor Required | Optional | Yes, must select one |
| Network Size | Typically larger | More focused/limited |
| Best For | Flexibility, travel, multiple specialists | Budget-conscious, local care, coordinated treatment |
For an in-depth look at Florida’s largest marketplace carrier, the Florida Blue review covers network size, pricing, and member satisfaction. Broader carrier rankings are available in the best health insurance Florida guide.
Understanding Health Insurance Costs in Florida for 2026
Florida marketplace premiums increased an average of 31.5% for 2026 before subsidies, according to the Florida Office of Insurance Regulation (FLOIR). After-subsidy costs increased even more significantly for many enrollees because the enhanced federal subsidies that had been in effect since 2021 expired at the end of 2025. Understanding both the sticker price and the after-subsidy cost is essential for accurate budgeting.

Sample Monthly Premiums: 40-Year-Old Individual, Before Subsidies
| Plan Type | Example Carrier | Monthly Premium | Deductible | Out-of-Pocket Max |
|---|---|---|---|---|
| HMO (Silver) | Health First | $645/month | $3,100 | $5,011 |
| EPO (Silver) | Cigna | $911/month | $2,208 | $5,476 |
| PPO (Silver) | Florida Blue | $1,510/month | $2,505 | $5,475 |
Note: These are sample rates for 2026. Actual costs vary by age, county, carrier, and specific plan. Subsidies significantly reduce these amounts for qualifying households.
📋 Real-World Scenario: How Subsidy Expiration Affects Costs
Maria, age 40, self-employed graphic designer in Miami-Dade County earning $22,590/year: In 2025, Maria paid $0 per month for her Silver HMO plan thanks to enhanced subsidies. For 2026, that same plan costs $81 per month—still affordable, but $972 more per year than before.
Roberto, age 60, earning $35,000/year in the same county: His 2025 plan cost $85 per month. For 2026, comparable Silver coverage runs approximately $485 per month—a $4,800 annual increase. Comparing all available carriers and plan types helped Roberto find a different plan that reduced this impact.
Compare Florida Health Insurance Plan Costs
Plan comparison based on specific doctors, medications, budget, and health needs reveals which options offer the best total annual value.
Compare All Plans Online Call 888-215-4045Detailed Plan Type Comparison for Florida Residents
This side-by-side comparison highlights the practical differences between the four main Florida health insurance plan types—HMO, EPO, PPO, and POS—across the factors that most affect daily healthcare experience and annual costs.
| Feature | HMO | EPO | PPO | POS |
|---|---|---|---|---|
| Primary Care Doctor | Required | Not required | Not required | Required |
| Specialist Referrals | Required | Not required | Not required | Required (in-network) |
| Out-of-Network Coverage | Emergency only | Emergency only | Yes, at higher cost | Limited, at higher cost |
| Relative Premiums | Lowest | Low–Moderate | Highest | Moderate |
| Administrative Hassle | Moderate (referrals) | Low | Low | Moderate (referrals) |
| Best For | Budget-focused, local care | Cost + flexibility balance | Maximum freedom, travel | Coordination + some flexibility |
How to Choose the Right Florida Health Insurance Plan
Choosing the best Florida health insurance plan involves balancing six factors: budget capacity, healthcare needs, provider network availability, prescription drug coverage, financial risk tolerance, and total annual cost projections. Following this step-by-step framework prevents the most common enrollment mistakes.
💰 Step 1: Set Your Budget
Determine what is affordable for both monthly premiums and unexpected out-of-pocket costs. Tight budgets lean toward Bronze HMOs; moderate budgets fit Silver plans; higher budgets support Gold or Platinum.
🏥 Step 2: Assess Healthcare Needs
Healthy individuals with rare doctor visits may benefit from Bronze or Silver. Those with chronic conditions, regular prescriptions, or expected procedures often save more with Silver CSR or Gold plans.
👨⚕️ Step 3: Verify Provider Networks
Confirm that current doctors, specialists, and preferred hospitals are in-network before enrolling. This is the single most important verification step—switching doctors mid-treatment creates disruption.
💊 Step 4: Check Drug Coverage
Review each plan’s formulary (list of covered drugs) to ensure current prescriptions are included. Check the tier placement—higher tiers mean higher copays—and whether prior authorization is required.
📊 Step 5: Evaluate Financial Risk
Those with limited savings benefit from Silver or Gold plans that cap unexpected costs. Those with substantial emergency funds may accept Bronze plan risk in exchange for lower premiums.
✅ Step 6: Calculate Total Annual Cost
Add 12 months of premiums plus expected out-of-pocket spending for 2–3 top plan options. The lowest-premium plan often costs more overall than a slightly higher-premium plan with lower deductibles.
Frequently Asked Questions About Florida Health Insurance Plans
These are the most commonly asked questions about Florida health insurance plans for 2026, covering plan type differences, enrollment deadlines, financial assistance eligibility, and provider network verification.
What is the difference between HMO and PPO plans in Florida?
HMO plans require choosing a primary care physician who coordinates care and provides referrals to specialists. Only in-network providers are covered except in emergencies. PPO plans allow seeing any doctor without referrals and cover out-of-network care at higher cost. HMO plans typically cost 20–40% less in monthly premiums than comparable PPO plans. Most Florida marketplace enrollees find HMO networks adequate for their needs and prefer the cost savings.
Which metal tier is the best value for most Florida residents?
Silver plans offer the best value for the majority of enrollees. They balance moderate premiums with reasonable deductibles, and they are the only tier eligible for Cost-Sharing Reductions—which can drop the deductible below $1,000 for individuals earning under $39,125 per year. Bronze suits healthy individuals who want the lowest possible premium and can handle a high deductible. Gold works better for those with chronic conditions or frequent medical visits.
Can Florida residents with pre-existing conditions get health insurance?
Yes. Under the Affordable Care Act, insurance carriers cannot deny coverage, charge higher premiums, or exclude benefits based on pre-existing medical conditions. This protection applies to all marketplace plans and ACA-compliant coverage sold in Florida. All 16 carriers participating in the 2026 Florida marketplace must accept all applicants regardless of health status.
What was the 2026 enrollment deadline for Florida health insurance plans?
Open Enrollment for 2026 ran from November 1, 2025, through January 15, 2026. Enrolling by December 15 secured a January 1 coverage start date. Enrollments between December 16 and January 15 started coverage on February 1. Outside Open Enrollment, coverage is available only through Special Enrollment Periods triggered by qualifying life events such as marriage, birth of a child, job-based coverage loss, or moving to a new area. Starting fall 2026, the enrollment window will shorten to November 1 through December 15.
How can Florida residents determine eligibility for premium tax credits?
Premium tax credits are available to individuals and families with household incomes between 100% and 400% of the Federal Poverty Level. For 2026, that means individuals earning $15,650–$62,600 or families of four earning $32,150–$128,600. The HealthCare.gov application calculates exact eligibility based on household size, income, and local plan costs. Cost-sharing reductions require Silver plan enrollment with income under 250% FPL ($39,125 individual, $80,375 family of four).
Can plan types or metal tiers be changed during the year?
No. Plan changes are only permitted during Open Enrollment or through a Special Enrollment Period triggered by a qualifying life event—such as job loss, marriage, having a baby, or moving to a new coverage area. Enrollees are locked into their selected plan type and metal tier for the full calendar year otherwise. Choosing correctly at enrollment avoids being stuck with mismatched coverage for 12 months.
Are EPO plans a good middle ground between HMO and PPO?
EPO plans offer HMO-level pricing without the referral requirement for specialists—a significant convenience advantage. The trade-off is no out-of-network coverage except emergencies. For Florida residents who stay in-network and want direct specialist access, EPO plans often deliver the strongest value: lower cost than PPO with more freedom than HMO. Verify that preferred providers are in the EPO network before enrolling.
How should doctor and hospital network coverage be verified before enrolling?
Each carrier maintains different provider networks, and these networks vary by plan type even within the same carrier. Before enrolling, specific doctors, specialists, and hospitals should be checked against each plan’s provider directory—available on the carrier’s website or by calling the carrier directly. Assuming a provider is in-network without verification is the most common source of unexpected medical bills after enrollment.
Florida Health Insurance Resources
How subsidies, tax credits, and cost-sharing reductions lower Florida coverage costs.
Best Health Insurance FloridaFlorida’s top carriers compared by cost, networks, service, and overall value.
Florida Blue ReviewIn-depth look at Florida Blue plans, pricing, network size, and competitor comparison.
Private Health Insurance FloridaPrivate medical insurance options with flexible benefits beyond the ACA marketplace.
Short-Term Health Insurance FloridaTemporary coverage for gaps between plans, including costs, limits, and eligibility.
Florida PPO PlansPPO health insurance plans offering flexible provider access and nationwide networks.
Find the Right Florida Health Insurance Plan
This guide covered Florida health plan types, metal tiers, carriers, costs, and how to evaluate options. The next step is comparing specific plans based on doctors, prescriptions, budget, and healthcare needs.
Get Free Quotes Call 888-215-4045Independent Broker Notice
ForHealthInsurance.com is an independent health insurance agency serving Florida residents. We are not affiliated with any carrier or government agency. We help you compare plans and enroll in coverage that meets your needs at no extra cost to you.